‘There’s no magic wand’ – GVMC officials speak out about decision to close labor & delivery unit

By Stephen Baldwin, RealWV
Dr. Connie Perkins is a 26-year veteran doctor in the Greenbrier Valley. As the lone obstetrician-gynocologist employed full-time by Greenbrier Valley Medical Center, she hasn’t taken a sick day in two years and has also been on call 20 days every month during that time.
“Back when we had three providers, we would deliver 600 babies a year,” she recalls.
“Through October of this year, we’ve delivered 218,” Becky Harless, Vice President of Vandalia Health and the administrator for GVMC, adds.
“It’s a national trend,” Perkins says. “The lack of providers here has also been a hit.”

Perkins works as part of a team along with two midwives, Sandra Cottle and Summer Hepler, a nursing team, and a rotation of visiting doctors who provide part-time coverage.
“We’ve reached the point,” says Perkins, “that it’s not sustainable.”
GVMC made the announcement that they were closing the labor and delivery unit in Spring 2026 earlier this month. It came as a shock across the Greenbrier Valley, with business leaders and moms alike decrying the decision as a blow to local quality of life.
Gov. Patrick Morrisey even scheduled a forum at the local medical school, the West Virginia School of Osteopathic Medicine, to distance himself from the decision. He said of the closure, “I don’t like it…It’s the opposite of what we’ve been trying to do. I want this to be a thriving community which means access to the services you need.”
Vandalia Health took over operation of the hospital in 2023, promising to increase locally-available medical services.
“By adding more doctors, more equipment, more staff at the hospital, more people can stay close to home when they’re ill and need our services.”
That’s what then-CEO of Vandalia Health Dave Ramsey said on January 1, 2023.
“There will be a huge difference in how the hospital is managed and cared for as an asset of the community. It is only focused on the well-being of the community, the services in the community and the health care that we can provide.”
Since then, Vandalia (the parent company of CAMC) has invested significant funding at GVMC in a new pharmacy, a revamped emergency room, new HVAC system, a medical records system, and a new multi-million dollar medical office building.
So why are they closing the labor and delivery unit?

“It’s three-fold,” Dr. Perkins says. “We just don’t have the staff…we haven’t been able to get the support from the ‘mothership’ (CAMC in Charleston) to fill in gaps…and the younger generation (of doctors) want a work/life balance.”
“We’ve tried to recruit,” adds Harless. “This place is like Hallmark at Christmas. We’ve taken them to dinner, showed them around town. There’s been issues with spouses not wanting to move here.”
“It’s also expensive,” Perkins says.
“Lynchburg closed their unit the same day we did,” Harless notes.

But a former doctor at GVMC questions the intensity of the recruitment efforts to find additional providers.
Dr. Samantha Chaffin was an OBGYN with GVMC from 2017-2023. Most of that tenure fell under the previous hospital owner, CHI. She left in mid-2023 as she said her requests for support to administration “fell on deaf ears.”
“We thought the switch to Vandalia was gonna improve things,” she says. “It really didn’t.”
Chaffin says she left over basic concerns about being unable to provide medically for her patients. “We hoped and wished and pleaded for on-call ultrasound services. That was very hit or miss and puts you between a rock and a hard place. Do you take this person to the operating room blind or transfer them out?”
“Also because we’re in a rural setting, we have limited blood products,” Chaffin says. “We don’t keep platelets in-house. I’m just painting a tiny picture of how being in a rural setting makes it trickier to practice here. Humans can only do so much.”
Chaffin says part of the reason GVMC has been unable to hire more providers is that the compensation package has not been adequate. “They didn’t make an enticing salary level offer, especially for someone coming to a rural area with limited ultrasound and blood products. We also have some of the highest malpractice insurance rates. If you’re gonna get someone to come to a rural setting and put their license on the line, you’ve gotta make it enticing. They did not.”
Baby deserts are a national trend
From 2017-2023, there were 217 labor & delivery units in hospitals nationwide that closed. A study by Harvard University’s School of Public Health pointed to several factors for the closure–declining birthrates, staffing shortages, increased costs, and the chilling effect of new antiabortion laws.
In addition, Professor Alicai McGregor found that “hospitals that appear most likely to close are often those most reliant on Medicaid.”
GVMC fits those categories as the region is in a population decline, struggles to recruit staff, faces increased costs like all health care providers, and a statewide abortion ban with very narrow exceptions was approved by West Virginia lawmakers in 2022.
At the time legislators were debating the public policy in 2022, Dr. William Artrip, who was then at GVMC, said, “It all has a negative influence on the health of West Virginians. It’s going to drive docs either to retirement or to drive them out of the state.”
The reason? Liability. Doctors fear being sued for trying to do their jobs in the midst of medical uncertainties.
The Association of American Medical Colleges reports one such example. “Mylissa Farmer, whose water broke prematurely, was told by emergency physicians in Missouri and Kansas that her fetus could not survive and she was at risk of bleeding and serious infection but that laws prohibited terminating her pregnancy, an amicus brief states. She wound up traveling four hours while in labor to receive necessary care.”
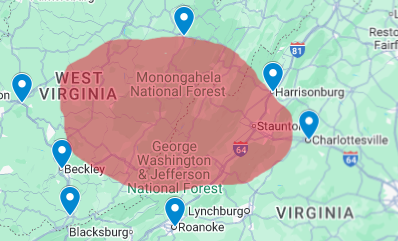
As the below map shows, the result is a so-called maternity care desert, where moms often have to drive long distances to deliver children. There are no labor and delivery services in the red bubble.
Molly McMillion is the Director of the WV Breastfeeding Institute and Special Projects Consultant for the WV Perinatal Partnership. She is a registered nurse who has worked with mothers and infants for nearly 30 years. She has seen eight hospitals stop offering deliveries in the last few years.
“I have taught childbirth classes here in the Greenbrier Valley for mothers delivering at GVMC and any of the surrounding hospitals,” McMillion shared. “There’s always a point in the class series that expectant parents realize that they must drive 1-2 hours away when in labor, and are terrified.”
“Greenbrier Valley ceasing to deliver babies next year is a loss to the community and a harsh reality for mothers,” she continued.
Perkins agrees, saying, “When you have a lack of service, you increase the risk something bad will happen.”
She says if an emergency room physician is faced with an emergency C-section, “They’re not trained for that.”
“With that being said, we’re not going to close and turn these moms loose,” Perkins pledges. “We’re in the process of talking to surrounding docs and their teams. Our moms don’t need to travel to Charleston for every visit. They can stay here, get care from us locally, then we’re clued into high risk pregnancies.”
Some have wondered if Perkins will continue practicing medicine locally, and she wants to clarify that she will. “I’m not retiring. I will be doing gynecology and prenatal work.”
‘No magic wand’

State and local politicians have floated the idea of providing incentives to increase the compensation package to attract local doctors to the area.
“I do understand the difficulty in recruiting,” says Delegate Ray Canterbury. “From the legislative perspective, we need to start finding ways to give incentives to serve in these kinds of critically underserved areas. Tax breaks or repaying student loans.”
Morrisey mentioned those possibilities in passing during his recent visit as well.
Becky Harless doesn’t believe those efforts will mark a turning point. “I’m concerned about false hope (in the community), like there’s this magic wand that’s gonna fix this.”
“It takes three people to replace Dr. Perkins,” she adds, saying they haven’t been able to recruit one OBGYN, let alone a team.
When asked if she had been able to talk to Gov. Morrisey since his visit, she replied, “Mr. Ramsey (the former CEO of Vandalia) has called the governor. We are still waiting on a call back.”
Perkins wishes she could continue delivering babies in her home community, but she says it’s just not sustainable. “I love my job, and I would continue doing OB if we had more helpers. I love our community. This is such a great place. We’re lucky. We’ve got a community of people that care. That’s why the outcry (against the closure) was so big. They care about each other.”
GVMC has also announced plans to reorganize as a “critical access hospital,” a financial decision tied to hospital reimbursement rates which will impact the emergency room and inpatient bed capacity. Stay tuned for additional reporting from RealWV on these issues in the coming weeks.



